Angiogram, As of currently diagnostic coronary angiography remains the primary component of cardiac catheterization. The aim is to examine the whole coronary tree (both native vessels and any bypass grafts) while recording details of the coronary anatomy, including the following, the pattern of arterial distribution, anatomic or functional pathology (atherosclerosis, thrombosis, congenital anomalies, or focal coronary spasm), and the existence of inter-coronary and intra-coronary collateral links.
The procedure Angiogram is usually performed in 30 minutes or less, under local anaesthesia, on an outpatient basis, with a procedure related significant complication rate (death, stroke, myocardial infarction) of < 0 . 1 %. It is possible to define all portions of the coronary arterial circulation down to vessels as small as 0.3 mm, free of any artefacts due to vessel overlap or foreshortening, by performing a series of intra-coronary contrast injections in fully chosen angulated views using current high-resolution x-ray imaging.
Protocol
Articles Needed for Angiogram
- Puncture needle (18 Gauge)
- Introducer wire .038′ Teflon (45cm)
- 6F sheath (12cm) with dilator
- 0.035′ Teflon guide wire (145cm)
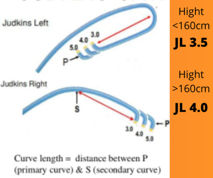
- Judkins Left 3.5 and Right Catheter 3.5 (6F)
Preparation
Ø Sterile Scrubbing, Gowning, Gloving
Ø Preparation Of Sterile Trolley
Ø Antimicrobial painting (from umbilicus to knee joint)
Ø Draping the patient in such a way that inguinal fold lies diagonal to the side hole
Ø Load 10ml of Xylocaine in 10 ml BD syringe and Heparin 2500 I.U in 5 ml BD syringe
Ø Flush the puncture needle, sheath, and dilator and Judkin’s Left and Right catheter.
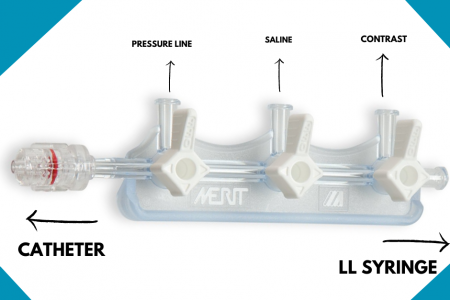
Ø Prepare manifolder
1. First port with Pressure line
2. Third port with contrast
3. Attach 10ml luerlock syringe
Procedure
Ø Puncturing femoral artery with puncture needle (18 G)
Ø Introducing 0.38′ Teflon introducer wire
Ø Removing puncture needle
Ø Making a small incision with scalpel blade
Ø Introducing the sheath with dilator
Ø Remove the dilator with wire & flush the sheath, Administer 2500 IU of Heparin
Ø Introducing LCA catheter with 0.035 Teflon guide wire
Ø Introduce the wire till it reaches the ascending aorta & hold the wire till the catheter reaches the ascending aorta then remove guide wire
Ø Aspirate 1 ml of blood in 5 cc empty syringe & flush the catheter with heparinized saline
Ø Connect manifolder to the catheter, Aspirate some blood & flush
Ø Open the pressure line & aspirate contrast
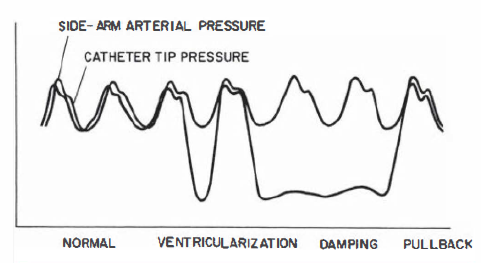
Ø Check whether the catheter hooks the coronary artery by giving small test injection and open the pressure line to check pressure damping.
Ø Inject contrast 4 – 5 ml for three cardiac cycle
Ø Introduce guide wire & remove the catheter
Ø Introduce RCA catheter with guide wire
Ø Once it is hooked, Give test injection then inject only 2-3 ml contrast
Ø For LIMA injection 5-6 ml of contrast to be injected
Ø For renal injection give 1 ml for each renal arteries
Ø Remove the catheter, sheath, check hemostasis & apply pressure bandage
Angiographic Views
The left coronary artery Angiogram
1 . RAO-caudal to visualize the left main, proximal LAD ,
and proximal circumflex
2. RAO-cranial to visualize the mid and distal LAD without
overlap of septal or diagonal branches
3. LAO-cranial to visualize the mid and distal LAD in an
orthogonal projection
4. LAO-caudal to visualize the left main and proximal
Circumflex
The right coronary artery Angiogram
l. LAO to visualize the proximal and mid right coronary
artery (RCA)
2. LAO cranial to visualize the distal right coronary artery
and its bifurcation into the posterior descending and
posterolateral branches
3. RAO-cranial to visualize the posterior descending and
posterolateral branches
4. Lateral to visualize the mid-RCA
Sheath Removal
Before trying to remove the sheath, confirm that the heparin is stopped, the activated clotting time (ACT) is less than 150 seconds, vitals are stable, no chest pain is present.
Remove the arterial sheath first if both arterial and venous sheaths were used, keeping excellent venous access in case the peripheral IV fails. Avoid putting pressure on the femoral vein for an extended period of time. Venous thrombosis can be caused by prolonged venous occlusion, especially when pressure devices are used. Check for cyanosis in the leg and foot.
Pressure holding time, which is usually 15–20 minutes, is determined by the sheath size, ACT, and difficulty of bleeding control.
